


In this issue, we look present a special report by an ICORD trainee who did an interesting project in Uganda, hear about brain plasticity, and talk about gender considerations in research. Plus: we tell you about some exciting new research studies, let you know what’s new at ICORD-O, and share some news from our partners.

by Ana Maria Oproescu
ICORD PI Dr. Lyndia Wu, with co-investigators Naznin Virji-Babul and Noah Silverberg, has been awarded a New Frontiers in Research Fund grant to study brain injury mechanisms in ice hockey players. Their new project proposes to monitor, in real-time, the head impacts sustained by ice hockey players, as well as their brain’s electrophysiological outputs, over the course of a playing season using wearable head impact sensors and EEG sensors. The project has two main objectives. First, Dr. Wu and her colleagues hope to use these real-time sensor technologies to better understand the elusive mechanisms underlying mild traumatic brain injury (mTBI), focusing specifically on cumulative damage from repeated subconcussive head impacts during sport. Second, this project will specifically address sex and gender-based differences in mTBI between male and female players, and will attempt to discern which factors might be causing these differences.
There’s a dearth of data on female athletes in contact sports within mTBI research (as many contact sports are male-dominant), but sex and gender differences in brain injury have been reported. For example, female players tend to sustain more head impacts at lower accelerations, but have more diagnosed concussions, worse outcomes and longer recovery times than male players. Therefore, such targeted analyses of sex- and gender-based differences are highly necessary.
For example, female players tend to sustain more head impacts at lower accelerations, but have more diagnosed concussions, worse outcomes and longer recovery times than male players. Therefore, such targeted analyses of sex- and gender-based differences are highly necessary.
“There’s a huge push on sex and gender analyses and considerations for any kind of studies of human biology,” says Dr. Wu. Sex-based (e.g. brain size/geometry) and gender-based (e.g. reporting behaviour) factors could both affect concussion outcomes, and Dr. Wu and her colleagues are carefully designing analyses that will compare both physiological parameters and social-psychological factors between male and female players.
“Teasing out these factors would help with different management or policy changes or game rule changes,” explains Dr. Wu. “If the difference arises from a difference in biology, where one sex has lower tolerance for brain injury given the same amount of force inputs to the head, then in that case we might need to change the helmet design to provide better protection. Or, if a particular sex is more vulnerable to cumulative brain injuries from multiple impacts, then maybe we’d need to further limit the amount of contact in that particular sex for better protection,” says Dr. Wu.
This two-year project is in its first phase of development. The team is currently designing the wearable EEG sensor (to ensure functionality and comfort for both sexes), as well as the gender-based factor investigation. Data collection will begin next year. The team hopes that, in addition to the highly accurate (eg. <10% error) wearable mouthguard sensors, the wearable EEG brain response sensors they are designing could be utilized in the future to provide continuous feedback on brain function during games. They also hope that their sex- and gender-based analysis will shed light on whether mTBI management should differ between male and female players.

Dr. Wu and her students work on the sensor
POST DOC OPPORTUNITY:
Dr. Wu is currently recruiting a postdoctoral researcher to assist in this work. Candidates with background in biomedical or mechanical engineering and expertise in instrumentation are preferred. Knowledge and experience in injury biomechanics, wearable sensing, or EEG would be a plus. Candidates are encouraged to contact Dr. Wu at lwu@mech.ubc.ca.

a special report by Graham Fronseca
 Worldwide, 90% of severe fractures occur in low and middle- income countries (LMIC). However, for medical staff in LMIC, there is no affordable and reliable solution to realign displaced hip and femur fractures intra-operatively. Existing solutions in high income countries are too expensive for most hospitals and medical centres in LMIC, ranging from $25,000 to $200,000. Without an affordable solution, medical staff turn to crude and unreliable methods, such as pulling manual traction, depicted in picture 1. Improper fracture fixation often results in permanent deformities and disabilities which do not allow patients to re-enter the workforce.
Worldwide, 90% of severe fractures occur in low and middle- income countries (LMIC). However, for medical staff in LMIC, there is no affordable and reliable solution to realign displaced hip and femur fractures intra-operatively. Existing solutions in high income countries are too expensive for most hospitals and medical centres in LMIC, ranging from $25,000 to $200,000. Without an affordable solution, medical staff turn to crude and unreliable methods, such as pulling manual traction, depicted in picture 1. Improper fracture fixation often results in permanent deformities and disabilities which do not allow patients to re-enter the workforce.
In order to address this problem, our team designed and constructed a traction device that can be manufactured for $1,000. It can reliably apply and maintain traction to an injured lower extremity for over one hour. It requires minimal training to operate, can be manufactured and serviced locally, disinfected after each use, and can be used in conjunction with mobile X-ray (C-arm).
We were lucky enough to travel to Uganda with the Uganda Sustainable Trauma Orthopaedic Program. Our trip began with a meeting hosted by Dr. Patrick Sekempi, Dr. Edward Kironde (surgeons) and Dr. Tito Beyeza (former head of orthopaedics) at Mulago Hospital. They not only gave us their blessing to use our device in surgery, but were enthusiastic about its potential impact. We then went straight to the Mulago Hospital Workshop (picture 2) to rebuild our device, as we had to ship it from Vancouver in pieces. Our last meeting of the day was with the local biomedical engineers from the University of Makerere whom we have partnered with to build a locally sourced device (pictures 3 and 4).
Throughout the first week, we were able to present our device to residents, years one through four, who are typically the ones providing manual traction during surgery. We received great feedback which will be incorporated into future iterations of our device. The most useful feedback, however, came from the surgeons themselves during surgery (picture 5).
The patient was a young woman who had just been admitted with a femur fracture from a gunshot sustained when a group of thugs tried to rob her store. She urgently needed irrigation, debridement, and stabilization of her femur. Our device was effective in reliably applying and maintaining traction and she is expected to make a full recovery.
After using our device in surgery, we held a closeout meeting with Dr. Patrick Sekempi. He suggested that he will use our device at least once a week on fresh fractures (up to two weeks old). He hopes that the medical staff will see patients recovering quickly which will get them onboard with reducing surgery wait times.
This project originated in the Engineers in Scrubs course. We are currently going through the Entrepreneurship @UBC program in order to determine a sustainable path for our device.
Team Members: Graham Fonseca, Dr. Kisitu Kyengera, Dr. Peter O’Brien, Dr. Jeff Potter, Andrew Schmidt, Dr. David Stockton and Justin Yu. Graham and Justin are both MASc students in ICORD’s Orthopaedic and Biomechanical Injuries Group. For more information about this project, please contact Graham

This year’s ICORD Loves Summer photo contest was won by PARC Coordinator Christine Hsin, who submitted this spectacular and inspiring photo of the PARC supervisors on a summer hike to St. Mark’s Summit. St. Mark’s Summit is a trail located near West Vancouver in Cypress Provincial Park with an incredible view of Howe Sound at the top. PARC Supervisors in the photo: Sharon Jang, Cameron Sihoe, Ariel Hung, Virgile Blais, Sarah Richter, and Christine Hsin.
See all the great entries here.

by Ana Maria Oproescu
ICORD researchers Corree Laule, Bonita Sawatzky, and Carolyn Sparrey are collaborating on a new study to investigate brain connectivity patterns in people with Amyoplasia, a congenital condition which impacts muscular development and growth. In Amyoplasia, the most common type of Arthrogryposis, an individual is born with weakened muscles and multiple joint contractures (from the feet sometimes up to the jaws). It’s currently believed that this condition is caused by dysfunctional cells within the anterior horn of the spinal cord (the region containing motor neurons that control our skeletal muscles).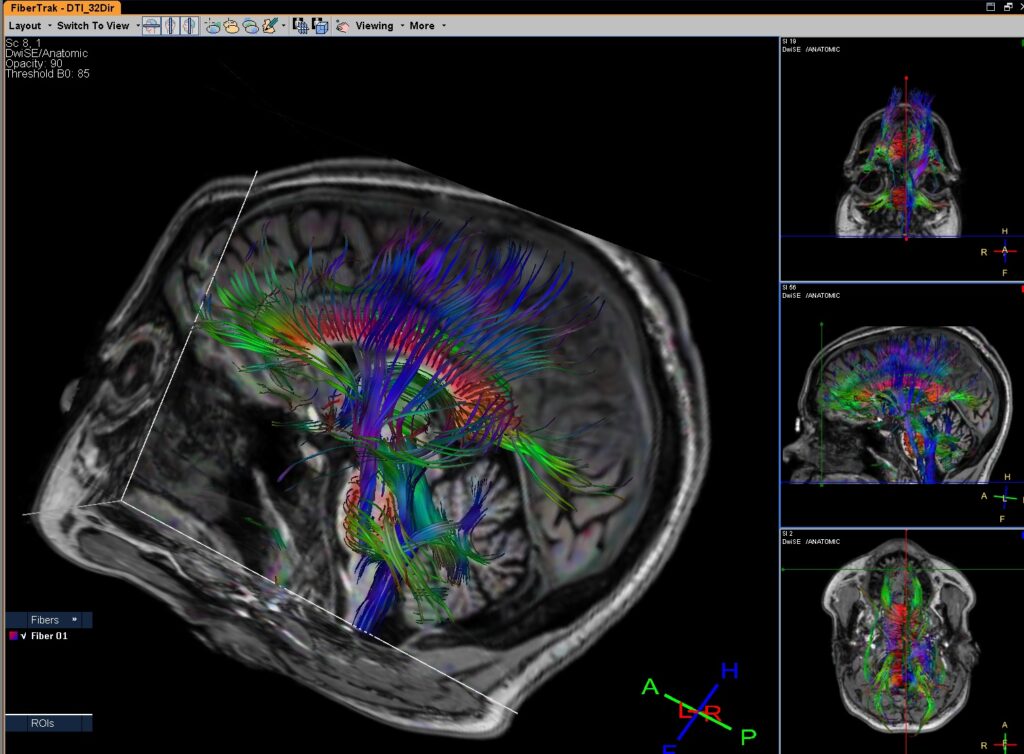 These dysfunctional cells are likely a result of an issue that occurs with the spinal cord’s blood vessels between 8-10 weeks of embryonic development.
These dysfunctional cells are likely a result of an issue that occurs with the spinal cord’s blood vessels between 8-10 weeks of embryonic development.
Using both magnetoncephalography (MEG) and magnetic resonance imaging (MRI) technologies, Drs. Laule, Sawatzky and Sparrey want to determine whether the brain’s connectivity adapts with such early damage to the spinal cord. They’re interested in the potential connectivity changes in the brains of children with Amyoplasia because these children demonstrate strong intellectual capabilities and are great problem-solvers. Despite their significant motor disabilities, previous research from Dr. Sawatzky’s lab has shown that children with Amyoplasia often end up pursuing post-secondary education, working, and getting married, similar to the able-bodied population.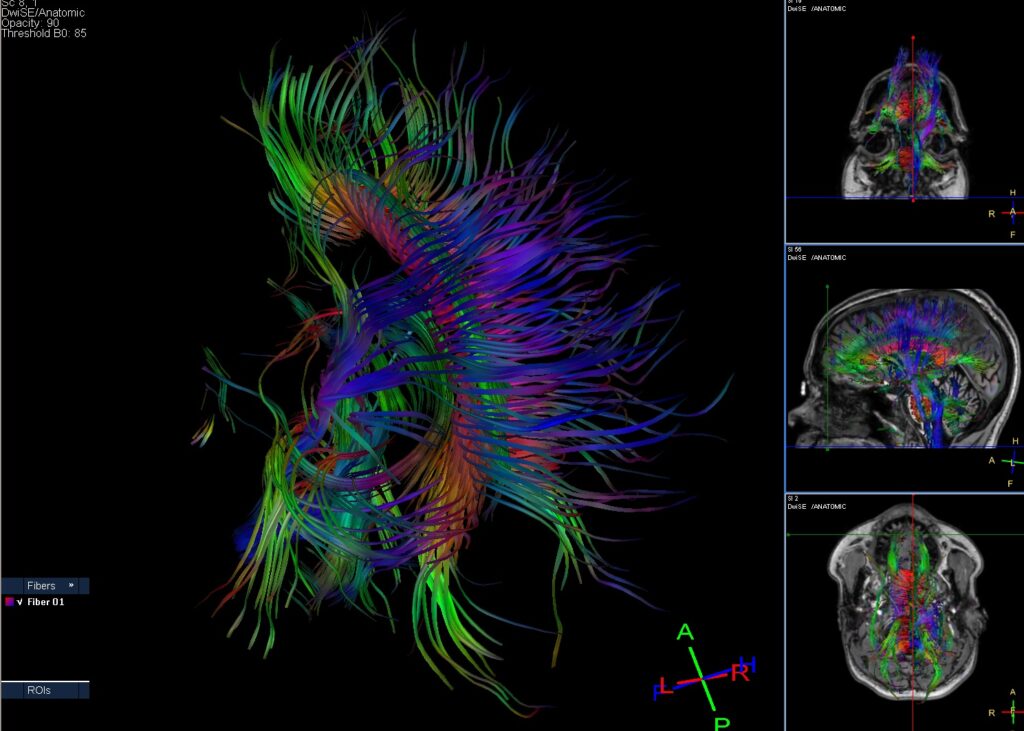
We know from previous research in the field of neuroplasticity that the brain can “rewire” itself, in response to injuries or environmental influences, to optimize its functionality. For example, research has shown that when the brain is deprived of one sense (for example, hearing loss), it can compensate with above-average function in another sense. This performance enhancement in the intact sensory system occurs by a process known as cross modal plasticity.
The researchers involved in this study are therefore interested in whether such plasticity occurs in the case of Amyoplasia. “Our research question is: what happens to the brain’s connectivity patterns when the motor cells of the cord are impaired? If the motor cortex so early on in development is not able to send motor signals down the cord as well as it should, does it pick up other “tasks” in the brain to do? Since it is adjacent to the prefrontal cortex, does the motor cortex region have greater connectivity to the prefrontal cortex allowing for more potential for problem solving tasks?” says Dr. Sawatzky.
This collaborative study is unique because, by combining MEG with MRI/fMRI technologies, the resolution of electromagnetic imaging can be significantly increased, and rapid neural processes and information pathways within the brain can be traced (which can’t be achieved using these technologies in isolation). MEG is a sensitive, high resolution test which picks up the brain’s electrical activity. MRI and fMRI, on the other hand, allow researchers to analyze the brain’s structure. So far the researchers have collected data on five individuals, and early data analysis is underway. The results of this analysis could inspire a host of follow-up investigations related to neuroplasticity after trauma to the central nervous system. If their study reveals connectivity changes or adaptations in the brains of individuals with Amyoplasia, then future research might also address neuroplasticity in children and adults with SCI.


Congratulations to PARC participants Sydney Spraggs (left), Mike Skelton (right), and Evelyn Legault (not pictured), who were part of the Off Balance dragonboat team that won gold at at the Steveston Regatta on August 24. Last year the same team won silver.

Some updates by Jan van der Scheer
A CIHR grant
ICORD PI Kathleen Martin Ginis, along with ICORD-O members Jan van der Scheer, Chris West, Kendra Todd and ICORD member John Kramer and other colleagues in Vancouver, has been awarded $554,624 by the Canadian Institutes of Health Research over three years to run a clinical trial on the effects of exercise on chronic pain in adults living with spinal cord injury.
A popular paper
ICORD-O members, together with their national and international collaborators, have won the Spinal Cord Readers’ Choice Award for best review paper published in 2018 for the paper Evidence-Based Scientific Exercise Guidelines for Adults with Spinal Cord Injury: An Update and a New Guideline. ICORD Authors include Kathleen Martin Ginis, Jan van der Scheer, Rob Shaw and Chris West.

Interested in helping ICORD researchers make SCI preventable, livable, and curable? These research studies (and more) are in need of participants!
![]()
Using virtual reality and eye-tracking to understand movement planning
Researchers in Dr. Tania Lam’s lab want to investigate how individuals with and without spinal cord injury (SCI) use their vision to plan a skilled walking task.
This study requires you to walk within a virtual reality environment using a specialized virtual reality headset that tracks your eye movements. During this study, you will be asked to approach and step over a virtual obstacle while attempting to deter an object in your peripheral vision. Watch the video below for a quick demonstration. Click here for details.
![]()
Comparing two ways of measuring pain
Researchers in Dr. John Kramer’s lab want to investigate whether people’s reported pain levels are impacted by different pain measures. They will induce mild levels of pain on your forearms using two different pain measurement protocols. To take part in this study, you must be between 18-45 of age and not suffer from chronic pain (pain lasting longer than three months) or a chronic disease. Click here for more information.
![]()
Male sexual functioning following SCI
Sexuality is a major rehabilitation priority and concern in men following SCI. Evidence from uninjured individuals demonstrates that physical activity can improve testosterone levels and certain health-related quality of life outcomes. However, it is unclear if physical activity has the same impact in persons with chronic SCI. In this study, Drs. Andrei Krassioukov and Stacy Elliott and their teams will investigate quality of life, sex hormone concentrations and perceptions of sexual function across two groups of men with SCI that perform different amounts of habitual, free-living physical activity. Click here for more information.
 Did you know that volunteers at our SCI Community Resource Centre prepare summaries of scientific papers and post them on our SCInfo blog? If you’re interested in what’s going on in SCI research around the world, this is a good place to look.
Did you know that volunteers at our SCI Community Resource Centre prepare summaries of scientific papers and post them on our SCInfo blog? If you’re interested in what’s going on in SCI research around the world, this is a good place to look.
We are excited to introduce a new series of web comics created by Adam Mesa. What topics would you like to see?

SCI BC wants you to know about
Multi-Sports Day
September 14, 10am- 3pm
Locarno Beach
Join the fun!
Virtual Peer Support
SCI BC has started a new playlist on our YouTube channel that includes videos from our online Peer Support groups on topic such as mindfulness, nutrition, research, etc. Here’s the playlist; check out one of the videos below.

Are you interested in growing your knowledge of accessibility? The recently launched Accessibility Professional Network connects professionals, students and those with an interest in accessibility in the built environment across the country, and brings critical resources to this growing group. Membership benefits include:
- Access to educational resources,
- Professional development and networking opportunities,
- Access to an industry job board,
- An online discussion forum,
- And more!
Membership is free until the end of 2019! Visit www.RickHansen.com/APN to join today.
The Network will also host its first annual conference Oct.31 – Nov.1, 2019 in Toronto. Those who register will get a free Network membership in 2020.


 ICORD and the Rick Hansen Institute are working together to identify new treatments for SCI and apply existing treatments for other neurological disorders, injuries and diseases to SCI. Funded by the Rick Hansen Foundation, the Blusson Integrated Cures Partnership provides ten years of stable funding for several multi-year research projects as well as new faculty positions within ICORD, international exchanges to encourage collaboration, research-related events (like the Annual Research Meeting and seminar series) and a consumer engagement strategy which aims to provide people with SCI and their supporters with evidence-based information about the healthcare, services and resources available to best support recovery after SCI and increase consumer involvement in the research process.
ICORD and the Rick Hansen Institute are working together to identify new treatments for SCI and apply existing treatments for other neurological disorders, injuries and diseases to SCI. Funded by the Rick Hansen Foundation, the Blusson Integrated Cures Partnership provides ten years of stable funding for several multi-year research projects as well as new faculty positions within ICORD, international exchanges to encourage collaboration, research-related events (like the Annual Research Meeting and seminar series) and a consumer engagement strategy which aims to provide people with SCI and their supporters with evidence-based information about the healthcare, services and resources available to best support recovery after SCI and increase consumer involvement in the research process.
We are very grateful for this generous support.
 Thanks for reading this issue of The ICORDian – we hope you enjoyed it! Please subscribe and have future issues delivered to your inbox. If you have any comments about this issue or suggestions for future ones, please contact us.
Thanks for reading this issue of The ICORDian – we hope you enjoyed it! Please subscribe and have future issues delivered to your inbox. If you have any comments about this issue or suggestions for future ones, please contact us.
 Ana Maria Oproescu, Adam Mesa, Graham Fonseca, Lyndia Wu, Jan van der Scheer, and Kent Niamath for their contributions to this issue of our newsletter.
Ana Maria Oproescu, Adam Mesa, Graham Fonseca, Lyndia Wu, Jan van der Scheer, and Kent Niamath for their contributions to this issue of our newsletter.


