Adrian Cheng, Lia Yu, Ana-Maria Oproescu
This is a summary of a research study done by Dr. Tania Lam and colleagues at ICORD. Dr. Lam’s research interests are focused on human walking and its relationship with the nervous system.
Click here to access to the original article, published in the Journal of Rehabilitation Research and Development.
How does body-weight support treadmill training help retrain walking?
Today, almost half of all people with spinal cord injury have some preserved voluntary motor function below their level of injury. This type of injury is called a “motor-incomplete” injury. Several studies have shown that with long-term, task-specific training, people with motor-incomplete injuries have the potential to recover basic walking functions.
Body-weight supported treadmill training (BWSTT) is an example of this type of rehabilitation training for people with motor-incomplete injuries. BWSTT uses a harness to support one’s body weight, while physiotherapists, treadmills, and robotic devices assist the person with walking movements. This assistance training can gradually re-train the nervous system to learn how to walk again. This type of rehabilitation training has also led to the development of a robotic device called the Lokomat, which automatically moves a person’s legs in uniform steps and eliminates the need of a physiotherapist to do this manually.
While BWSTT has gained significant attention in walking rehabilitation training for people with SCI in recent years, there is no strong evidence suggesting it is more effective than simple overground walking training. The researchers in this study wondered if a more challenging training program, which utilized “feedback-error learning” (a type of motor learning) would be more effective in improving skilled walking. Put simply, in this learning scheme, our cerebral cortex compares our desired movements with our actual movements. If it detects an error by sensory feedback, it instructs the cerebellum to alter the motor command to make the actual movement more closely resemble the desired movement.
Previous studies have shown that exposure to forces that resist movement during walking lead to longer stride lengths once the forces are removed, via a process of feedback-error learning. Similarly, this study focused on whether or not applying a resistance force on a person’s leg as they tried to walk could lead to greater improvements in motor control once the force was removed. ICORD researchers wanted to determine whether applying a resistance force during BWSTT would be a more feasible and effective rehabilitation method than regular BWSTT to teach those with motor-incomplete spinal injuries how to walk again.
Who took part in the study?
Individuals with motor-incomplete spinal cord injury were tested in this study. Participants needed to be able to walk on a treadmill with body weight support, but without any manual assistance.
How were the participants tested?
Participants were randomly assigned to one of two groups. Participants in the first group (experimental group) were trained with BWSTT and exposed to resistance forces against their hip and knee by the Lokomat device. The researchers controlled the magnitude of the force. The second group (control group) was trained with the conventional Lokomat-assisted BWSTT, without resistance forces applied.
Each participant trained for 45 minutes, three times a week for three months, under supervision of the ICORD researchers. Researchers tested the subjects at baseline, post training, and after the one month and six month follow-up marks.
The outcomes that the researchers measured in both groups were related to overground skilled walking capacity (i.e. tasks encountered on a daily basis). Skilled walking capacity was tested by the “Spinal Cord Injury-Functional Ambulation Profile” (SCI-FAP).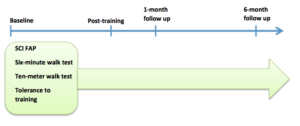
Other tests included a ten-meter walk test (how fast an individual can walk this distance), and a six-minute walk test (how far an individual can walk in this time). Researchers also kept a record of the participants’ tolerance to the training they did, in order to assess the feasibility of the training program.
What did the researchers find?
For the simple walking speed and distance tests, both the control and experimental groups showed the same amount of improvement from their different training programs. However, the experimental group showed significantly improved performance compared to the control group in overground skilled walking tasks during their post-training and follow-up assessments. This is an interesting finding, as it suggests that treadmill training, with the added challenge of resistance forces, can mimic the aftereffects of more challenging and dynamic overground training, during which participants explicitly practice different walking skills. The improvements in skilled walking after the resistance-applied BWSTT program indicates that generalization is occurring in the participants’ motor learning: they have improved in skills and contexts that they didn’t specifically train. Participants who underwent walking rehabilitation with these applied forces against their hip and knee were engaged in a feedback-error process, which allowed them to transfer the effects of learning from the Lokomat-resisitance device, to an overground setting. The results from this pilot study suggest that a robotically-applied resistance can be useful to patients who have suffered from a motor-incomplete spinal cord injury to improve their walking skills beyond the skills they specifically train during the program.

